Cutting Edge Techniques
Cone Beam CT Scanner
Dental cone beam computed tomography (CT) is a special type of x-ray machine used in situations where regular dental or facial x-rays are not sufficient. This type of CT scanner uses a special type of technology to generate three-dimensional (3-D) images of dental structures, soft tissues, nerve paths, and bone in the craniofacial region in a single scan. Images obtained with cone beam CT allow for more precise treatment planning.
With cone beam CT, an x-ray beam in the shape of a cone is moved around the patient to produce many images, also called views. CT scans and cone beam CT both produce high-quality images.
Cone beam CT provides detailed images of the bone and is performed to evaluate diseases of the jaw, dentition, bony structures of the face, nasal cavity, and sinuses. It does not provide the full diagnostic information available with conventional CT, particularly in the evaluation of soft tissue structures such as muscles, lymph nodes, glands, and nerves. However, cone beam CT has the advantage of lower radiation exposure compared to conventional CT.
Common uses of the Cone Beam CT Scanner?
Dental cone beam CT is commonly used for treatment planning of orthodontic issues. It is also useful for more complex cases that involve:
- surgical planning for impacted teeth
- diagnosing temporomandibular joint disorder (TMJ)
- accurate placement of dental implants
- evaluation of the jaw, sinuses, nerve canals, and nasal cavity
- detecting, measuring and treating jaw tumors
- determining bone structure and tooth orientation
- locating the origin of pain or pathology
- reconstructive surgery
*information pulled from Radiologyinfo.org
CO2 laser
The advantages of the CO2 Laser are a relatively bloodless surgery, decreased postoperative discomfort, minimal swelling and scarring, and the laser’s ability to coagulate, vaporize, or cut. The CO2 surgical laser offers the dental surgeon a viable and in many cases an improved alternative to the scalpel. The CO2 laser system is a useful tool in a wide variety of soft-tissue oral laser surgery procedures. A laser beam (instead of a scalpel) is used to assist with the list of oral surgery applications below:
- Frenum release/frenectomy
- Abscess (drainage)
- Flap surgery
- Biopsy (incisional & excisional)
- Aphthous ulcers (incision & excision)
- Excision & ablation of lesions, benign & malignant lesions, oral cavity tumors, and hemangioma
- Salivary gland pathologies
- Preprosthetic gum preparation, leukoplakia
- Partial glossectomy
- Periodontal gum resection
- Homeostasis
- Operculectomy
- Crown lengthening (soft tissue)
- Incision of infection when used with antibiotic therapy
- Extraction site hemostasis
Guided Implant Placement
Guided implant surgery is the process of planning the implant surgery on a computer using the patient’s CBCT image. We work with a lab to generate a virtual representation of the patient’s jaw and oral anatomy. This is utilized to develop a digital treatment plan in which the exact position of the implant is determined in advance of treatment. A surgical guide is fabricated by a lab that controls the osteotomy in precise accordance with the preplanned implant position.
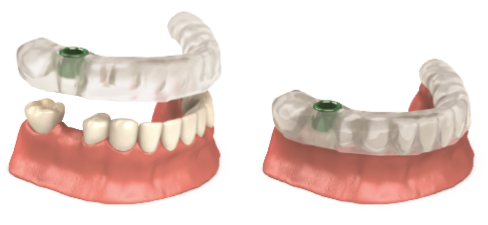
Image of an implant guide
Pros for Guided Implant:
- Surgery can be precise, safe, and predictable.
- Surgery time is shorter.
- Generally carried out as a flapless surgery and shorter recovery time for the patient.
- Less invasion, blood, and pain for the patient.
- Immediate loading is possible.
- Bone grafts can be minimized.
Downside for Guided Implant:
- It is more expensive due to working with the lab to fabricate the guide.
Platelet-rich plasma (PRP)
Platelet-rich plasma (PRP) is a new approach to tissue regeneration and is becoming a valuable adjunct to promote healing in many procedures in dental and oral surgery, especially in aging patients. PRP derives from the centrifugation of the patient’s blood and contains growth factors that influence wound healing, thereby playing an important role in tissue repairing mechanisms.
The use of PRP in surgical practice could have beneficial outcomes, reducing bleeding and enhancing soft tissue healing and bone regeneration. Studies conducted on humans have yielded promising results regarding the application of PRP to many dental and oral surgical procedures (i.e. tooth extractions and implant surgery). The use of PRP has also been proposed in the management of bisphosphonate-related osteonecrosis of the jaw (BRONJ) with the aim of enhancing wound healing and bone maturation. The aims of this narrative review are: i) to describe the different uses of PRP in dental surgery (tooth extractions and periodontal surgery) and oral surgery (soft tissues and bone tissue surgery, implant surgery and BRONJ surgery); and ii) to discuss its efficacy, efficiency and risk/benefit ratio. This review suggests that the use of PRP in the alveolar socket after tooth extractions is certainly capable of improving soft tissue healing and positively influencing bone regeneration, but the latter effect seems to decrease a few days after the extraction.
PRP has produced better results in periodontal therapy in association with other materials than when it is used alone. Promising results have also been obtained in implant surgery, when PRP was used in isolation as a coating material. The combination of necrotic bone curettage and PRP application seem to be encouraging for the treatment of refractory BRONJ, as it has proven successful outcomes with minimal invasivity. Since PRP is free from potential risks for patients, not difficult to obtain and use, it can be employed as a valid adjunct in many procedures in oral and dental surgery. However, further RCTs are required to support this evidence.
Piezosurgery
Piezosurgery is a promising, meticulous, and soft tissue-sparing system for bone cutting, based on ultrasonic microvibrations. The main advantages of piezosurgery include soft tissue protection, optimal visibility in the surgical field, decreased blood loss, less vibration and noise, increased comfort for the patient and protection of tooth structure. To date, it has been indicationed for use in oral and maxillofacial surgery, otorhinolaryngology, neurosurgery, ophthalmology, traumatology, and orthopedics. The main indications in oral surgery are sinus lift, bone graft harvesting, osteogenic distraction, ridge expansion, endodontic surgery, periodontal surgery, inferior alveolar nerve decompression, cyst removal, dental extraction, and impacted tooth removal. In conclusion, piezosurgery is a promising technical modality for different aspects of bone surgery with a rapidly increasing number of indications throughout the whole field of surgery.
*information pulled from NCBI

CBCT guided jaw surgery
CT Scan Guided Surgery involves the use of three dimensional CT imaging to better visualize the patient’s bone without having to surgically expose the area.
Based upon the findings of the CT Scan, a treatment plan of the implant operation is made using specialized computer software on the CT Scan. This information is then transferred to a computer-generated surgical template which guides the implant instrumentation exactly to the desired location in such a way that it matches the treatment plan and turns it into reality.
The procedure starts by having the dentist fabricate a radiographic guide which is essentially a set up of the patient’s ideal teeth in acrylic. If the patient’s denture has the teeth in their ideal position, the denture may be used as the radiographic guide. A CT scan of the patient’s bone, as well as the radiographic guide, are then performed. This CT scan allows for the generation of a three-dimensional model of the jawbone and the proposed teeth that can then be used in virtual reality software to plan the implant placement. Once the implant positions and sizes are determined and planned, the software then generates a special guide from this planning that may be used for 2 purposes: 1) to perform the surgery in a minimally invasive fashion 2) to fabricate the fixed teeth that are placed on the implants right after the surgery
Guided surgery provides a link between the surgeon’s plan and the actual surgery. It also has several important enhancements and advantages over conventional surgeries. First, the patient and the surgeon are better prepared for what they will encounter during the procedure. Complete information about the quality and quantity of the bone makes it possible to determine the ideal location for the implants that enhance the final esthetic outcome, while also avoiding important anatomy in the area. This translates into fewer complications and surgery time is often decreased. Because many surprises are eliminated by the enhanced treatment planning, treatment costs are also more predictable.
Horizontal & Vertical Ridge Augmentation
Bone morphogenetic protein (BMP)
BMP is an isolated protein that induces specific cells in our body to form new cartilage and bone. During surgery, the BMP is soaked onto and binds with a collagen sponge. The sponge is then designed to resorb, or disappear, over time. As the sponge dissolves, the bone morphogenic protein stimulates the cells to produce new bone. The BMP also goes away once it has completed its task of jump starting the normal bone healing process.
Since there is no need to harvest bone from the patients’ hip for BMP, recipients were spared donor site pain. Complications from the graft harvest site are also eliminated with the use of bone morphogenic protein.



